Expert Perspective: This authoritative guide is presented by Professor Seungho Baek. By synthesizing clinical pathology with proactive longevity strategies, Prof. Baek provides deep insights into the biological mechanisms of Osteoporosis Prevention Key Factors.
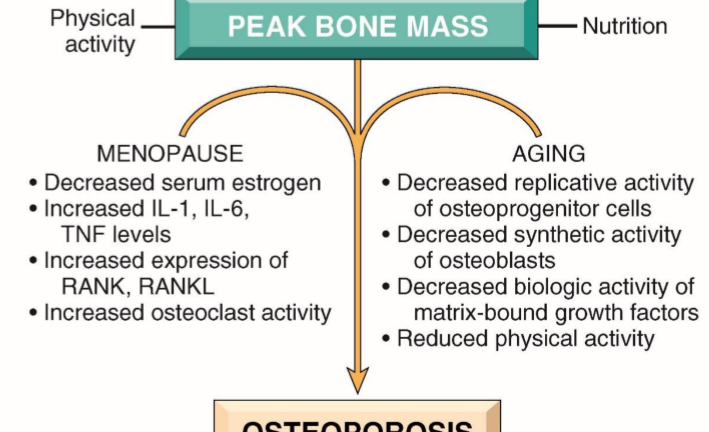
Osteoporosis is a systemic skeletal disorder characterized by diminished bone mass and increased fracture risk. Professor Seungho Baek identifies physical inactivity as the primary modifiable risk factor. Biologically, bone tissue adheres to the “use it or lose it” principle; without muscular load, osteoblast activity diminishes. Effective Osteoporosis Prevention Key Factors include maximizing peak bone mass before age-related decline and understanding how cellular responses to growth factors change in the aging bone matrix.
Osteoporosis is often described as a “silent thief” because bone loss occurs without symptoms until a fracture happens. As Professor Seungho Baek, I emphasize that understanding Osteoporosis Prevention Key Factors is not just about clinical management—it is about decoding the biological signals our bodies send to our skeletal system.
1. The Spectrum of Bone Loss: Osteopenia to Osteoporosis
Before addressing prevention, we must understand the progression. Osteopenia is the initial decrease in bone density. When this loss reaches a threshold where structural integrity is compromised, it is diagnosed as Osteoporosis.
This condition can be localized (such as disuse osteoporosis following an injury) or widespread, affecting the entire skeleton. As we age, managing Osteoporosis Prevention Key Factors becomes essential to prevent fragility fractures and vertebral compression that can lead to permanent disability.
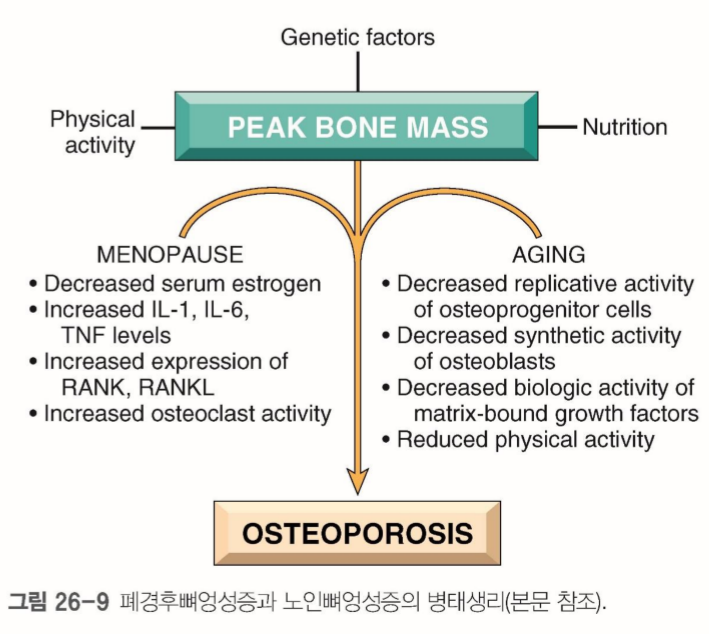
2. The Primary Modifiable Factor: Physical Activity
Among the various Osteoporosis Prevention Key Factors, one stands out as entirely within our control: Physical Activity. While genetics and aging are inevitable, our movement patterns provide the mechanical load necessary for bone remodeling.
“Professor Seungho Baek Insight: Bones exist to support muscles. When physical inactivity becomes chronic, the body perceives no biological demand to maintain high bone density. This metabolic efficiency—discarding what isn’t used—is the root cause of many cases of preventable osteoporosis.”
In developed nations, the lack of mechanical loading (gravity and muscle pull) is a significantly larger contributor to bone mass loss than simple nutritional deficiency. Nutrition supports the process, but physical demand triggers it.
3. Aging and the Cellular Microenvironment
Aging is an inevitable process that reduces bone mass by approximately 0.7% per year after peak density is reached. However, Professor Seungho Baek notes that the cellular quality of the bone changes alongside its quantity.
At the cellular level, older adults experience:
- Reduced Osteoblast Proliferation: Bone-building cells divide less frequently.
- Diminished Biosynthesis: Cells produce less of the extracellular matrix.
- Growth Factor Resistance: Bone cells become less responsive to repair signals.
4. Skeletal Adaptation and the Biology of Belief
Aligning with the principles in The Biology of Belief, our skeleton responds to the “environment” of our lifestyle. If we perceive ourselves as fragile, our cells enter a “conservation mode.” By choosing an active, strong perception, we send a “survival signal” that maintains osteoblast activity even into late seniority.
5. Conclusion: 7 Pillars of Osteoporosis Prevention
To summarize Professor Seungho Baek’s guide to Osteoporosis Prevention Key Factors:
- Early Resistance Training: Maximize peak bone mass before age 30.
- Mechanical Loading: Use weight-bearing exercises to stimulate osteoblasts.
- Consistent Mobility: Prevent disuse osteoporosis by avoiding prolonged sedentary behavior.
- Hormonal Monitoring: Pay close attention to bone density during postmenopausal transitions.
- Growth Factor Support: Maintain a metabolic environment conducive to cell signaling.
- Balance and Coordination: Exercise to prevent falls.
- Proactive Screening: Use early osteopenia as a call to lifestyle action.